By Tom Orrell, Consultant, Global Partnership for Sustainable Development Data; Managing Director, DataReady
Imagine that you were in charge of monitoring the effectiveness of a whole national health system. That it was your responsibility to know, at any given time, which diseases were causing the most deaths, in what numbers, where, and to whom. Your colleagues in other parts of the health ministry, including the minister, request frequent data on the top killers – from acute pandemics like COVID-19 to chronic epidemics like HIV/AIDS. Imagine that it was your job to provide the data that in turn enabled everyone else in the Ministry of Health to do their jobs effectively. That you were providing the fuel that enabled each person and department to work together as an engine propelling a whole country towards the promise of universal healthcare (UHC) – a promise Kenya’s government committed to achieve by 2022 as part of its “Big 4 Agenda” – and better health outcomes for all.
This is the position that Dr. Joseph Sitienei, Head of the Department of Health Sector Monitoring in Kenya’s Ministry of Health, finds himself in. Data is his lifeblood. Dr. Sitienei needs a constant stream of data to flow from health facilities across Kenya’s 47 counties into his department. However, instead of one constant stream of data, the situation more closely resembles a mishmash of data tributaries, all flowing in different directions. Some people are double counted, while others are not counted at all. Documentation gaps exist where some records are digitized but others remain paper-based, and there are often time lags in the reporting of key health metrics.
From Dr. Sitienei’s perspective, achieving UHC will require having the right data in the right hands at the right time, so that he can support his colleagues’ work. But with many data streams flowing from many sources across the health sector, it is imperative that the data are interoperable – joined-up in such a way that the data retains its contextual meaning but can be automatically processed, aggregated, and integrated with other data by a computer.
For the past year, the Global Partnership for Sustainable Development Data (the Global Partnership) has been supporting Dr. Sitienei in his quest to join-up health sector data in Kenya by:
- supporting the Ministry’s efforts to finalize and operationalize the Kenya Health Information Systems Interoperability Framework (“the interoperability framework”) ; and,
- focusing on the interoperability of HIV/AIDS-related data in Kenya, curated by the Ministry of Health’s National AIDS and STI Control Program (NASCOP) and the National AIDS Control Council (NACC).
As the projects draw to a close, we can reflect on how it has contributed to strengthening heath systems and attaining UHC. To do this, this piece describes the enabling policy environment in Kenya before reflecting on progress being made in the HIV/AIDS sub-sector, and finally considering how Kenya’s new health data interoperability framework helps to lay the foundations for future health system strengthening.
Harmonizing policy objectives: interoperability in the health sector
Joining-up data systems is not just a technical task. To be useful, joined-up data has to be relevant to the people and entities that need it most. This means involving all relevant stakeholders in the planning, implementation, and monitoring of e-health system design to bring together the range of organizational and individual workflows and objectives. At a ministry-wide level, this requires ensuring that foundational policy frameworks are in place that clarify the strategic objectives of e-health for various stakeholder groups and provide everyone with incentives and sense of ownership in their implementation.
The need is particularly acute in Kenya given the decentralized approach to healthcare provision. Authority and decision-making over health system strengthening activities are divided between national government and the 47 counties; and healthcare is dispensed through a combination of public, private, and faith-based providers.
Kenya coherently and consistently recognizes the need for health data interoperability from a legislative level all the way down to operational guidance. To support the integration of data streams flowing from each part of the country, the Health Act 2017 explicitly mandates a “mechanism for ensuring inter-connectivity between each county’s information systems.” This legal provision is then elaborated on in the Kenya National e-Health Policy 2016 – 2030, and the Kenya e-Health Strategy. Building on these, the Global Partnership helped develop the interoperability framework and its commensurate roadmap (discussed further below), which provide operationalizable details for health sector stakeholders.
To complement the Ministry’s robust policy framework, Dr. Sitienei Chairs the Health Information System Inter-Agency Coordination Committee (HIS ICC). The HIS ICC is a multi-stakeholder forum that convenes periodically to coordinate and take decisions on health informatics, health metrics, and research and innovation; the three pillars of the e-Health Strategy. Interoperability between data systems has always tacitly been a part of the HIS ICC’s mandate. With the finalization of the interoperability framework, which elaborates on the terms of reference of the ICC’s technical working groups to explicitly include interoperability at various junctures, the final piece of the policy puzzle is in place and the central importance of interoperability as an enabler of data exchange, integration, and aggregation has been affirmed.
Connecting health datasets and dashboards: HIV/AIDS data management
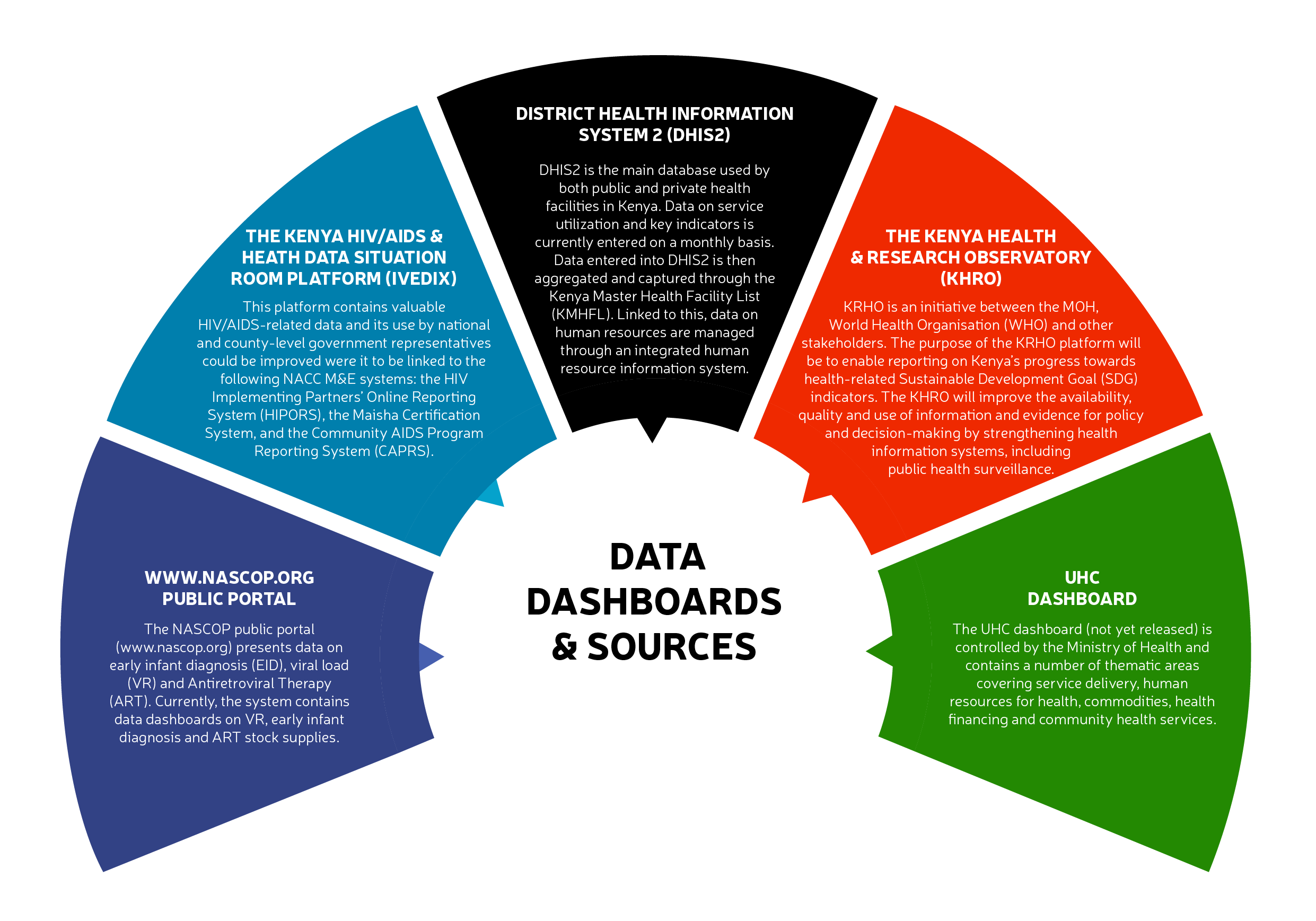
In recent years, the Ministry of Health, NASCOP, and NACC have invested in the development and deployment of several data dashboards and platforms that host HIV/AIDS-related datasets (see Figure 1 above). Monitoring progress against development targets including national targets, relevant SDGs, and the UNAIDS 90/90/90 targets to control the AIDS epidemic by 2020 is particularly complex. This is due to the range of interventions that are needed to achieve them – starting with preventative programmes such as girls’ education, access to diagnostics and anti-retroviral therapy (ART); as well as treatments for the multitude of HIV-related co-morbidities. While data exist for these indicators, they are fragmented, with gaps across Kenya, which is enhanced by uneven progress in e-health system development across the country’s 47 counties.
As part of the Global Partnership’s work with the Ministry of Health over the past year, the following two learning exercises were undertaken to better understand the opportunities to join-up HIV/AIDS-related data in Kenya to help inform policy interventions.
Firstly, the Global Partnership and The United States President's Emergency Plan For AIDS Relief (PEPFAR) commissioned a study of good practices and lessons learned from the PEPFAR-managed DREAMS partnership – a package of preventative interventions that holistically supports adolescent girls and young women at risk of HIV/AIDS – in Kenya, Uganda and Zimbabwe. As a participant country, Kenya operates a DREAMS database, which provides decision-makers across health, social services, education, and other service sectors with access to data, from a range of sources, pertaining to vulnerable adolescent girls and young women in the country via a safe and de-identified web-based portal. Access to this joined-up data highlights how data can help to provide public health decision-makers, who are often quite far removed from day-to-day efforts to combat HIV/AIDS, with contextually rich data that adds nuance to their work. Given the priority attached to achieving UHC in the near future in Kenya, creating a more nuanced, coherent, streamlined, and accessible set of HIV-AIDS data platforms and dashboards has become a higher priority for planners within the ministry, including Dr. Sitienei. The DREAMS database provides an excellent early example of what can be achieved.
Secondly, the Global Partnership, the Ministry of Health, and the NACC conducted a detailed assessment of the issues that are currently impeding more widespread interoperability between key datasets and systems in the HIV/AIDS sub-sector. This helped the NACC in particular to understand where to focus efforts to join-up the multiple datasets that feed into their day-to-day work (see Figure 1). When it comes to enabling interoperability between datasets across computer systems, issues that might seem innocuous to the human eye can become difficult to process for computers in an automated way. For example, the District Health Information System (DHIS2) is an open source data system that enables health facilities across the country to feed data into Kenya’s HIV Situation Room data dashboard. However, different health facilities update their DHIS2 datasets at different time intervals, which can create distortions in the insights that are then gleaned from the data. It can also result in dataset duplication.
“We now understand the challenges we are facing. There is no shortage of health information systems in Kenya. What we need to do is to bring the systems together to enable timely and accurate decisions to be made. The key to this will be creating synergy between strategic information (SI) teams and the IT department at the NACC. SI teams know what they want but IT knows the limitations and trade-offs involved in providing data and how accessing data retrieved at a certain point in time might affect analytics at a later date.
Moving forward, we need a change management mechanism within the NACC that can help SI teams to understand the repercussions for data analysis if - for instance - we change the parameters for age data disaggregation at the point of data entry. Ultimately, I believe we can now find approaches to interoperability that work both technically and for decision-making.”
George Onyango, Systems Administrator from the NACC
Laying the foundations for universal healthcare in Kenya: The 2020 interoperability framework
The examples above highlight how crucial joined-up data is for the decision-making needed to tackle complex health crises such as the HIV/AIDS epidemic. They also highlight the difficulties and opportunities inherent in making data interoperable; in particular, the puzzle of technical, data-related, individual, and organizational factors that need to align to create operational and useful systems.
Kenya’s new Health Information Systems Interoperability Framework was designed to tackle these challenges comprehensively at a national level. Building on Kenya’s strong e-health policy foundation, the framework is the product of a year’s worth of coordination, convening, and consultation work. The approach reflects the Ministry of Health’s recognition of the organizational and human dimensions of interoperability and the paramount importance of ensuring that e-health policy keeps apace of technical developments to ensure that all parts of the health system have a stake in data systems at each point in the value chain.
In many respects, this project’s unique focus on engagement and coordination is reflected in the framework itself, which emphasizes governance and leadership as key enablers of joined-up data. Moreover, implementation of the framework is designed to slot into existing policy coordination mechanisms within the Kenyan health sector. The document sets out the terms of reference for the various technical working groups established under the remit of the HIS ICC. In this way, it specifies how interoperable data can facilitate the attainment of better health outcomes by connecting data that decision-makers need at different levels of the health system in more structured, timely, and complete ways.
For Dr. Sitienei, HIV/AIDS is one epidemic within a much broader patchwork of health issues. By implementing the framework, the country can start to move towards more targeted health interventions.
“Through the President’s Big 4 Agenda there is a currently an unprecedented political moment in Kenya to really change health delivery in the country. As it stands, different parts of the health system define ‘health information’ differently. At the health facility level, health information refers to statistical aggregates. For doctors and nurses, it is patient-specific. For lab technicians it means test results. What we need to do is to join-up all of these interpretations and ensure that the data they imply is joined-up to form a holistic picture of the country’s health needs. This will require moving beyond just capturing service statistics towards patient-level data in the form of electronic patient records and electronic medical records. This approach will then allow for much more detailed and specific data analysis that captures the context and nuance of healthcare needs in the country.
The interoperability framework provides one of the foundational cornerstones for us to progress towards this vision. It provides the Ministry with a clear mandate and roadmap on how we can start to get all the streams of health data in Kenya all flowing in the same direction, unified in purpose.”
Dr. Joseph Sitienei, Head, Department of Health Sector Monitoring, Republic of Kenya Ministry of Health

